My Diagnosis With An Invisible Disease Called, “POTS”
~ Dysautonomia Awareness ~
https://linktr.ee/ashley_liermann
Spread the word for awareness, support, and learn more at the main foundations: https://www.dysautonomiainternational.org/

https://www.standinguptopots.org/

Invisible diseases are just as important as any other health-related problem that affects a person, and way of living. A person that may look normal and healthy on the outside could really be battling just to make it through another day. These illnesses range in many forms, but are considered invisible as the person may not always show external signs or symptoms.
Some symptoms of those living with an invisible illness or disability can include pain, fatigue, dizziness, weakness, or mental disorders. Examples of some conditions include diabetes, heart disease, dementia, autoimmune disorders, and even cancer. The list is broad in this category.
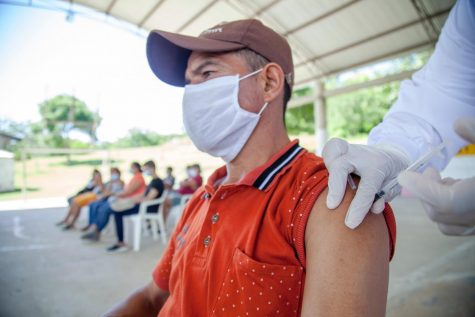
Today, I’m sharing part of my personal diagnosis and answering questions of an invisible disease called, “POTS.” It falls in the category type of an autoimmune disorder – also called, “Dysautonomia.”
In hopes to bring more awareness for all who are battling just to make it through another day, and in hopes that if you’re reading this and are a person struggling with this condition or any illness of sorts, that you’re not alone. You’re stronger than you know, and there are still many good people who care and want to provide resources to help you.

What is Dysautonomia?
According to the President of Dysautonomia International, Lauren Stiles stated,
“Dysautonomia is the most common condition you’ve never heard of, and maybe it’s what is dragging you down.”
Stiles goes on to explain in the interview how on average it takes patients nearly five years and longer to be properly diagnosed due to lack of awareness.
Dysautonomia is a broad term for many different medical conditions that cause problems with the autonomic nervous system (ANS) and keep it from functioning together properly and normally.
The ANS controls involuntary functions we don’t “consciously” think about like your heartbeat, blood pressure, body temperature, breathing, and digestion.
There are different forms of dysautonomia, and this is used as an “umbrella” term to refer to your nervous system functions.
A most common form that falls under this umbrella term is called Postural Orthostatic Tachycardia Syndrome – also known as POTS.
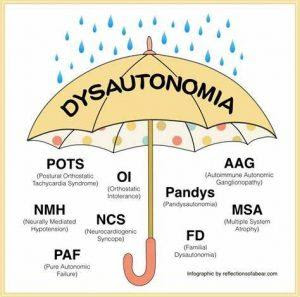
What is POTS?
POTS is a form of dysautonomia that stands for, “Postural Orthostatic Tachycardia Syndrome.”
Hopkins medicine defines it as this:
Postural: related to the position of your body
Orthostatic: related to standing upright
Tachycardia: increased heart rate
Syndrome: a group of symptoms
Hopkins medicine also says “POTS is a common condition affecting an estimated one to three million Americans.”
Which I’ve never heard about until one day, I ended up in the ER and was finally diagnosed with an answer that several doctors couldn’t give me before and am currently battling it day to day now.
This is a disorder that causes problems with the blood flow and can cause your heart to beat too fast when you stand.
The development of symptoms that come when standing up from a recline position may be relieved by sitting or lying back down. Heart rate and blood pressure work together to keep the blood flowing at a healthy pace no matter what position a person is in.
With POTS – Hopkins medicine says it is also defined as, “A heart rate increase from horizontal to standing (or as tested on a tilt table) of at least 30 beats per minute in adults, or at least 40 beats per minute in adolescents, measured during the first 10 minutes of standing.”
It also says, “Some people with POTS can develop hypotension (a drop in blood pressure) with prolonged standing (more than three minutes upright). Others can develop an increase in blood pressure (hypertension) when they stand.”
Meaning when I stand or change positions, my heart rate and body is doing triple the amount of work than compared to a normal healthy person.
People with POTS can’t keep a steady and stable blood pressure, but people diagnosed with this can range in different severities.
I cannot tell you the exact date that having POTS started for me. It is possible that I may have had it my entire life and never really known until circumstances triggered it into making it chronic and finally, noticeable. Symptoms and feeling unwell that grew progressively worse day by day with no answers until that day in the ER.
Next I’ll be talking more about those symptoms, how it affects a person, and how it varies.

What are some symptoms of POTS?
According to the Dysautonomia International Foundation, “more than 70 million people have dysautonomia,” and “POTS estimated impact between 1million and 3million Americans and many more around the world.”
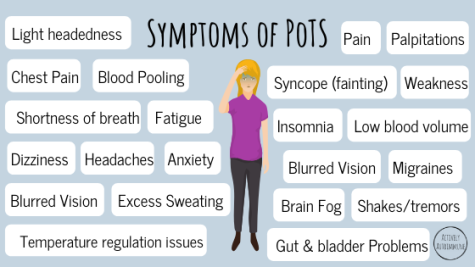
Some symptoms of POTS can include:
– Light-headedness and dizziness (worsens upon standing or even prolonged sitting)
– Presyncope (feeling of going to faint, but without actual loss of consciousness)
– Fainting (symptoms vary from person to person, but some do faint with prolonged sitting or standing)
– Chronic pain
– Fatigue
– Fast heartbeat and heart palpitations
– Chest pain
– Brain fog
– GI problems (such as bloating, and nausea)
– Shortness of breath (can feel breathless upon standing or slight exertion)
– Shakiness (tremors)
– Poor sleep
– Red-ish legs upon standing
– A variety of many symptoms
Some Known Triggers That Can Make Symptoms Worse:
– Heat
– Menstrual cycle
– Dehydration
– Alcohol
– Exercise
– Standing or sitting for a prolonged time
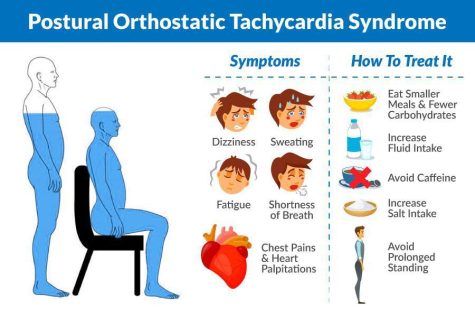
What causes POTS?
Both Hopkins medicine and Dysautonomia International say, “researchers don’t fully understand the cause of POTS as many diseases and conditions can cause it” however have a partial list of known conditions that can cause POTS such as: traumas, surgery, vaccinations, anemia, infections, diabetes, and more.
Every case and person is different and the entire underlying causes that brings on POTS is not entirely known. A few triggers that are known to develop POTS are:
– Surgery
– Trauma (such as head injury)
– A viral illness
– Serious infections
– Pregnancy
An example they include is that cases of POTS are increasing in people who have recovered from COVID-19 from having the infection, yet the body continues to experience symptoms for months after being called, “long-haulers.” It affects the heart rate and blood pressure.

For me, I have had symptoms of lower blood pressure than normal and extremely cold hands even when it’s over 100 degrees outside ever since I was younger. Followed by being diagnosed with “anxiety” and generally not feeling my best starting in middle school. I went through a phase that I missed a lot of school because of it that greatly impacted my life. I had to eventually switch to independent studies because I wouldn’t have graduated with my class if I didn’t make a change from missing so much. I was still able to be very active though, able to function through, and have a good positive attitude in moving forward. I even worked multiple jobs while doing school.
This makes me believe now thinking back that I could have had Dysautonomia/POTS without even knowing.
1 Common Question: “Is POTS caused by anxiety?”
According to Dysautonomia International,
“while some physical symptoms of POTS overlap anxiety, such as tachycardia and palpitations – POTS is not caused by anxiety and is often misdiagnosed as having anxiety or panic disorder and research has shown that POTS patients are less likely to suffer anxiety or panic disorder than the general public”
For me, my symptoms became chronic and more after a trauma in an accident on a water park slide that smashed my head and body in 2018.

That’s when the journey really began in seeking continuous treatments to be better. I was no longer able to work my retail job as it was too physically demanding. I was too ill with chronic pain, dizziness, and being sick to barely get out of bed. I eventually underwent jaw surgery for it as well as dental surgery with treatment in hopes to help relieve and fix some of the pain and problems I experienced. It helped for a while but not completely, as I continued being seen by many doctors with little answers still.
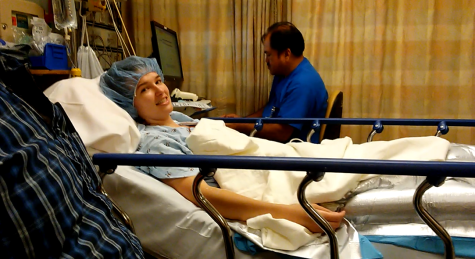
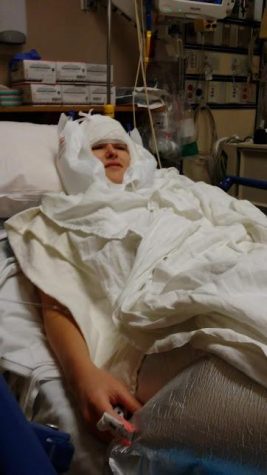
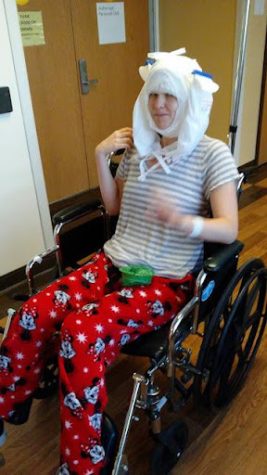
Fast forward 3 years later to the day in 2021 that I was finally diagnosed with POTS at a trip to the ER. All the days prior leading up to the trip were very difficult as each day I continued declining in my health and not knowing why. This happened to the point that I could no longer walk normally or even stand anymore. I hung onto walls and relied on things close to me to prevent falling and quickly sit from the feeling of going to pass out, tremors, chest pain, heart racing, dizziness, etc. I knew in my instincts that it wasn’t just anxiety I was having, as many tried to claim. Something more is going on.

I can tell you it was a relief to finally have some kind of answer that day at the ER and to know I wasn’t going crazy, as it felt I was from everything. It was more scary not knowing before with the many symptoms I had. Knowing now makes it less scary, but it is still a challenge in facing them indeed.
Quality of life and is it fatal?
Dysautonomia International says,
“Physicians with expertise in treating POTS have compared the functional impairment seen in POTS patients to the impairment seen in chronic obstructive pulmonary disease (COPD) or congestive heart failure. Approximately 25% of POTS patients are disabled and unable to work. Researchers found that quality-of-life in POTS patients is comparable to patients on dialysis for kidney failure.”

Although they say POTS is not life threatening, it *is* very life *alternating.* It’s about finding a new normal in doing things a bit differently than others and being sure to take care of oneself.




Above are some pictures of me before the accident, before my diagnoses, and severity of symptoms. I still had symptoms prior, but I was able to still function and be active whereas now it is a challenge to do everyday activities and find new ways to do things.
The biggest risk for people with POTS is falling and injuries from the added trauma. Some people with POTS even faint, but keep in mind that not all do, and rather feel faint and dizzy.
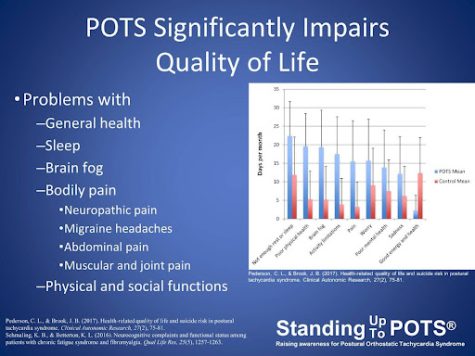
Some patients with mild symptoms can continue with normal work, school, social, and activities while for others, severe symptoms make normal daily activities severely limited, even standing and walking. Severity in cases is different in every person and what works for them in managing symptoms, some being bedridden while others can do more activity.
Next, I’ll talk about ways that are recommended in helping to manage POTS.
Diagnosed:
Several tests may be performed in order to rule out any other conditions such as anemia, vitamin deficiencies, heart conditions, etc.
Oftentimes, patients with dysautonomia and POTS tests will come back normal–as far as blood work, ekg’s, etc. This is why they go so long without a proper answer as to why they are not feeling well accompanied by having a wide variety of many symptoms yet tests state normal.
Some specialists that often diagnose dysautonomia and further management are cardiologists and neurologists.
The most common test to diagnose POTS is called the “tilt table test” or “poor man’s tilt test” which checks vitals of heart rate and blood pressure from lying, sitting, and standing positions.
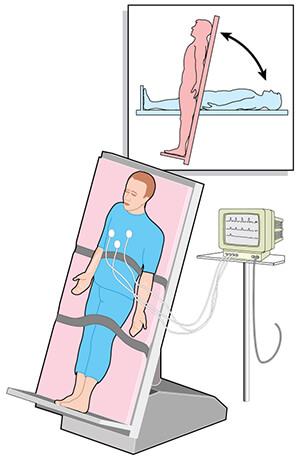
Other tests they may perform can include wearing a holter monitor to monitor the heart rate over a course of time.
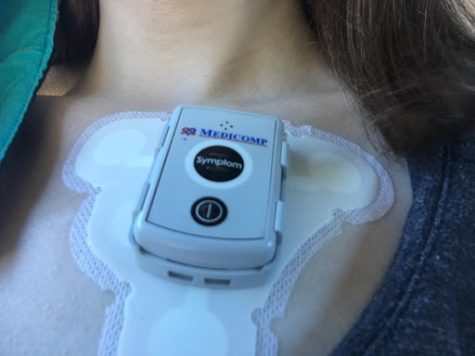

Treatments:
Currently, there is no known cure for dysautonomia and POTS, but rather ways in managing symptoms. The key to managing POTS is finding what triggers symptoms worse for a person – keep in mind that each person is different in severity and what works for them. It’s also important to note and remember that not all patients faint that have it, but rather feel faint and dizzy and generally not well from the nervous system not working as it should.
Most commonly recommended ways to help manage it, and for POTS includes:
– Increasing sodium (3,000mg – 10,000mg per day)
– Minimum 80oz water per day (more if it’s hot outside or doing more activity)
– Electrolytes
– Wearing compression stockings
– Small and frequent meals with salty snacks in between
– Medications may be prescribed to help manage different symptoms , but there is not a FDA approved medicine for this condition
– Lifestyle changes (diet, building up intolerance to exercise)
It is a process of finding out what works for the person and avoiding triggers that can make symptoms worse.

Helpful Mobility Aids:
Due to being unable to stand for long periods of time, some may need aids to help in assisting, such as seats, canes, walkers, wheelchairs, and more. At the moment, I use a walker with a seat that helps enable me to do my daily tasks. The seat is helpful in allowing me to be able to sit down and act like a wheelchair while still being able to work my legs and walk the little I can in a day. Without it, I’d most likely be bedridden due to the severity of my symptoms. It helps in preventing falls and getting hurt.





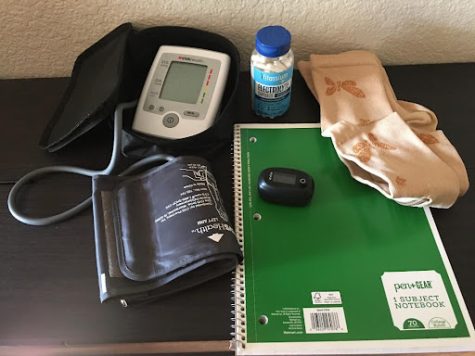
Other Helpful Devices and Tips:
Other devices that some may find helpful are at home blood pressure machines and heart rate monitors to help keep track of when symptoms may be worse or triggered. Keeping a notebook and writing down notes can help in finding a balance in managing.
Conclusion:
It is important to bring awareness and be aware of those with Dysautonomia and POTS in hopes to find a cure, better treatments, and overall, having a supporting and positive community around.
This applies to everyone in treating all with kindness and letting each other know that you’re not alone in whatever you may be facing in life and that circumstances don’t define who you are. You still have a choice to make the best of things where you’re at and be thankful for the little things in each day despite any challenges.
You never know what another person might be going through, even if they look “normal” on the outside. You can look at me and see that I look “normal,” but I am battling day to day, hour to hour. This form of dysautonomia disease is called POTS, which can also be known as an “invisible disease” because you don’t always see it physically.
Though it is hard to handle sometimes, it motivates me more to try my best, keep moving forward, and not remain quiet, but rather share to help others that may be going through the same, or worse. You’re not alone and you’re a part of the community in every way. I’d like to leave you with one of my many favorite quotes that took a whole new meaning to me in these times by Martin King Jr.
“If you can’t fly then run, if you can’t run then walk, if you can’t walk then crawl, but whatever you do, you have to keep moving forward.”

Sources:
30 things about living with postural orthostatic tachycardia syndrome (POTS). Sweatpants & Coffee. (2019, September 18). Retrieved from https://sweatpantsandcoffee.com/30-things-about-living-with-postural-orthostatic-tachycardia-syndrome-pots/
Blaylock, A. J. (2019, December 4). Dysautonomia: ‘most common condition you’ve never heard of’ is why you may feel lousy. firstcoastnews.com. Retrieved from https://www.firstcoastnews.com/article/news/local/dysautonomia-most-common-condition-youve-never-heard-of-is-why-you-probably-feel-lousy/77-833e7d65-4d40-4ad3-9b3d-b113a651f48c
Dysautonomia international: Dysautonomia awareness, dysautonomia advocacy, dysautonomia advancement. Dysautonomia International: Dysautonomia Awareness, Dysautonomia Advocacy, Dysautonomia Advancement. (n.d.). Retrieved from https://www.dysautonomiainternational.org/
Dysautonomia: Symptoms, causes, types, & how to live with. Cleveland Clinic. (n.d.). Retrieved from https://my.clevelandclinic.org/health/diseases/6004-dysautonomia
Goodreads. (n.d.). A quote by Martin Luther King Jr.. Goodreads. Retrieved from https://www.goodreads.com/quotes/26963-if-you-can-t-fly-then-run-if-you-can-t-run
Marcella. (2017, December 21). How to support those with invisible illnesses. Northwest Primary Care. Retrieved from https://www.nwpc.com/supporting-people-with-invisible-illness/
Postural orthostatic tachycardia syndrome (POTS). Johns Hopkins Medicine. (n.d.). Retrieved from https://www.hopkinsmedicine.org/health/conditions-and-diseases/postural-orthostatic-tachycardia-syndrome-pots
-pots
Direct Links:

Hi there! I’m Ashley L.
I call myself a ~ Positively Creative Dreamer ~ because I love being creative in all forms with hopes to inspire and bring...